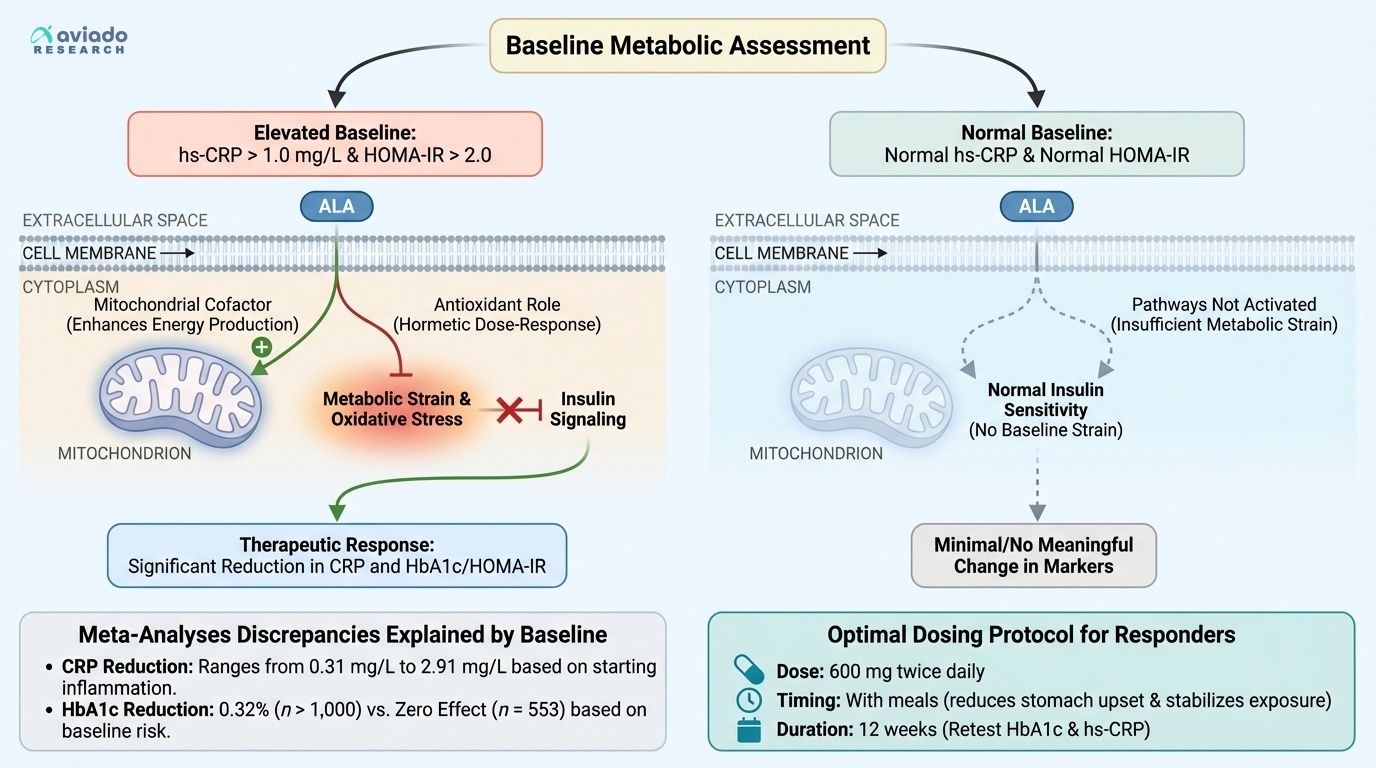
Even among responders, ALA's benefits extend beyond blood sugar control. A 12-week study found that ALA supplementation reduced VCAM-1, a marker of blood vessel inflammation, by approximately 2 ng/ml [11]. This vascular protection may be particularly important for people with metabolic syndrome, who face elevated cardiovascular risks.
Liver health represents another area where ALA shows consistent benefits. A 12-month trial combining ALA with ursodeoxycholic acid found significant improvements in liver enzyme levels [12]. While this study used combination therapy, it suggests ALA may support liver function in people with metabolic dysfunction, where fatty liver disease is common.
These broader effects make sense given ALA's role as a mitochondrial cofactor. Tissues with high energy demands—like the heart, blood vessels, and liver—may be particularly responsive to improvements in cellular energy production, especially when metabolic stress is already present.