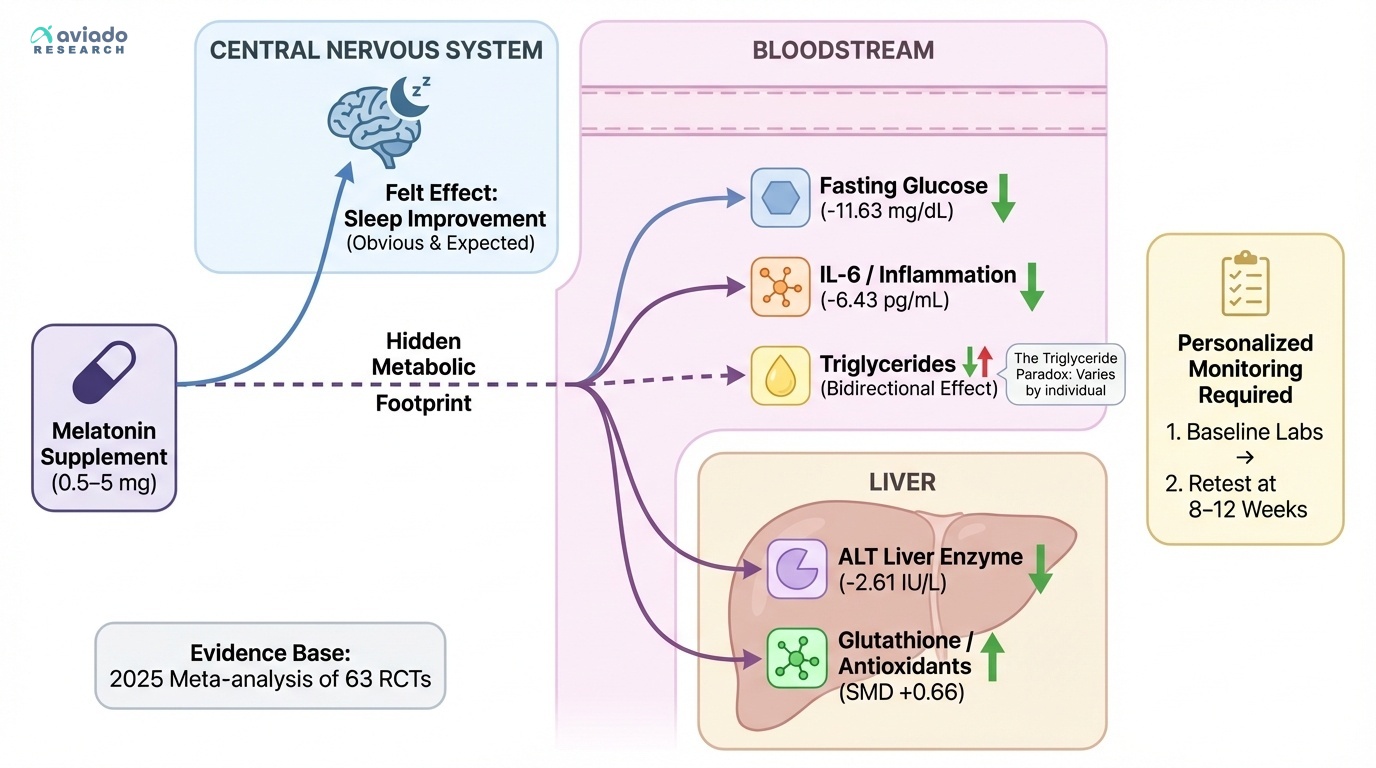
While melatonin's effects on liver enzymes and antioxidant systems are remarkably consistent, its impact on lipid metabolism reveals a more complex picture that highlights the importance of individual monitoring. Some studies show triglyceride levels decreasing with melatonin supplementation, while others document increases, creating a bidirectional effect that population averages can mask.
This variability suggests that melatonin's metabolic effects may depend on individual factors like baseline health status, genetic variations in melatonin metabolism, or concurrent medications and supplements. The same 3-5 mg dose that improves inflammatory markers in one person might simultaneously worsen lipid profiles in another, making personal biomarker tracking essential for determining net benefit.
The triglyceride paradox exemplifies a broader principle in personalized supplementation: population-level research can identify average effects, but individual responses often vary significantly from these averages. This is particularly relevant for melatonin because its metabolic effects are "silent"—they don't produce noticeable symptoms the way sleep improvements do. Without regular lipid panels, users have no way to know whether their melatonin regimen is providing metabolic benefits or creating biochemical changes that could impact cardiovascular health over time.