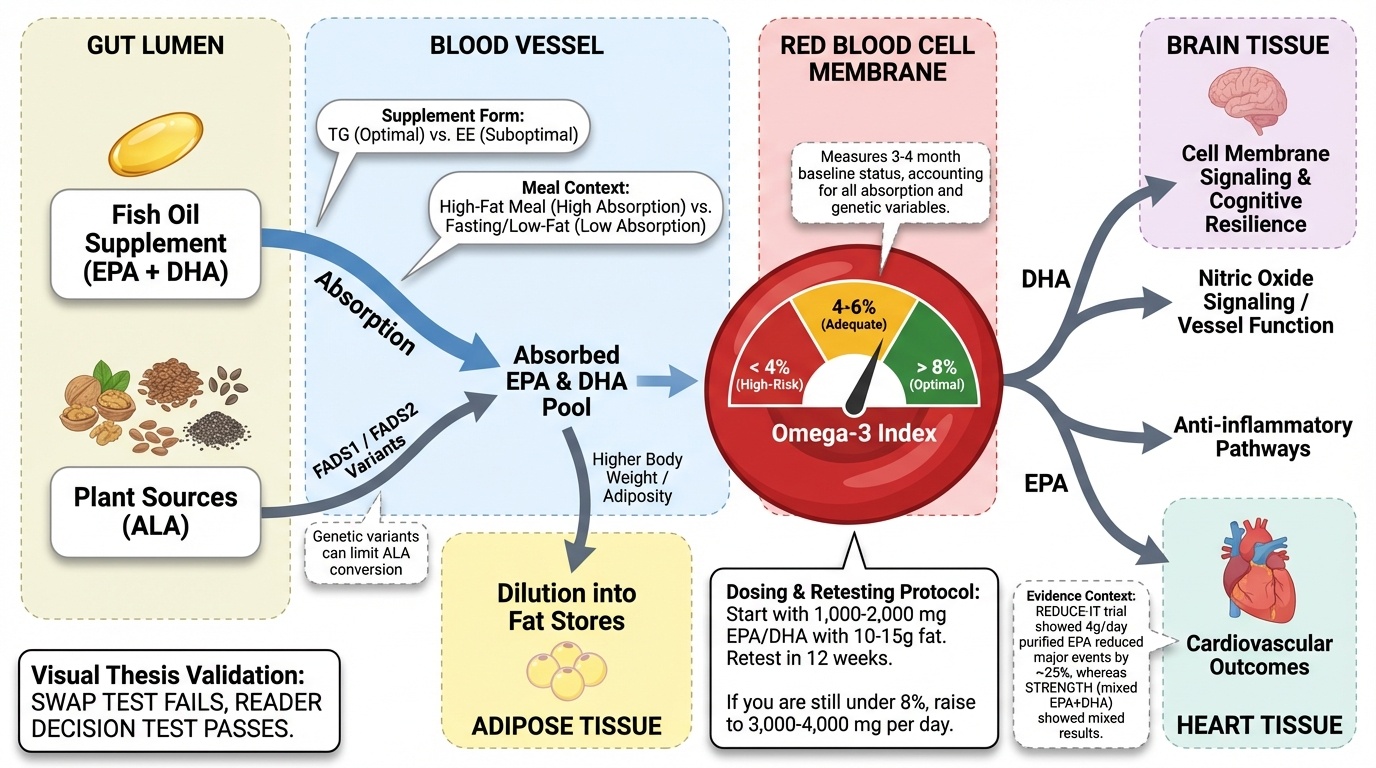
Two people taking identical 1,000 mg fish oil capsules can end up with different blood levels of EPA and DHA, the active omega-3 fatty acids. Studies show that health outcomes track with achieved blood levels rather than supplement doses, with individual variation in absorption and metabolism affecting how much EPA and DHA reaches the bloodstream from a given dose.
The omega-3 index—a blood test measuring EPA and DHA as a percentage of total red blood cell fatty acids—measures actual omega-3 status rather than supplement intake. Research suggests an optimal range of 8-12% for cardiovascular protection, though most omega-3 index research has focused on cardiovascular outcomes with less data for other health goals.
The evidence is clearest for triglyceride reduction, which shows dose-dependent responses that correlate with achieved blood levels rather than capsule amounts. Meta-analyses examining omega-3 supplementation find that effects on triglycerides and inflammation markers relate more closely to plasma concentrations than to supplement doses, though the relationship varies by baseline health status and individual factors.