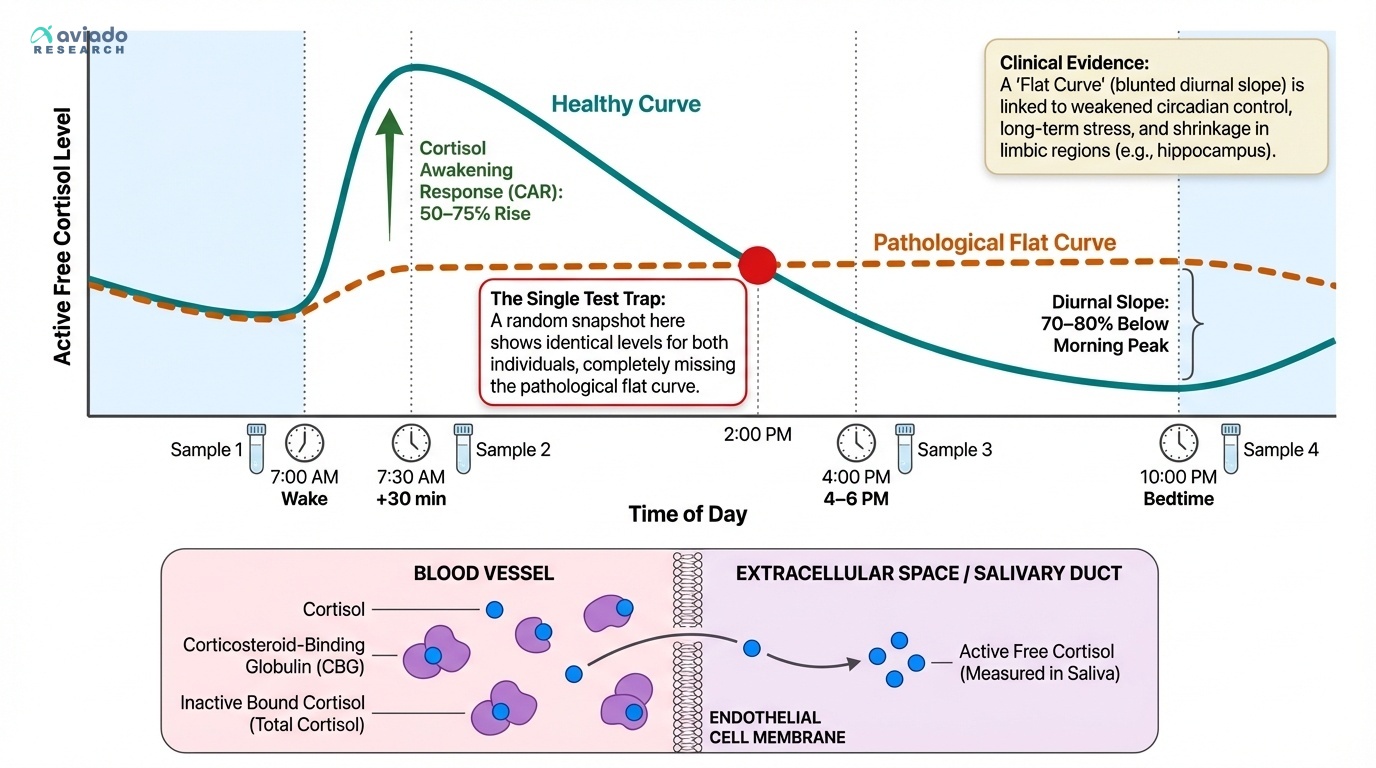
The surprising truth is cortisol is not one number. It is a daily rhythm. Most people test once. They panic. But the time of day can fool you.
This means you should measure your pattern. Not a single value. Your healthy day looks like this. High after waking. Then it falls all day. If it stays high at night, your sleep can suffer.
Use a 4-point saliva test in one day. Sample at wake time, then 30 minutes later. Sample again at 4–6 PM. Sample again at bedtime. Aim for a 50–75% rise after waking. Aim for bedtime levels 70–80% below your morning peak.