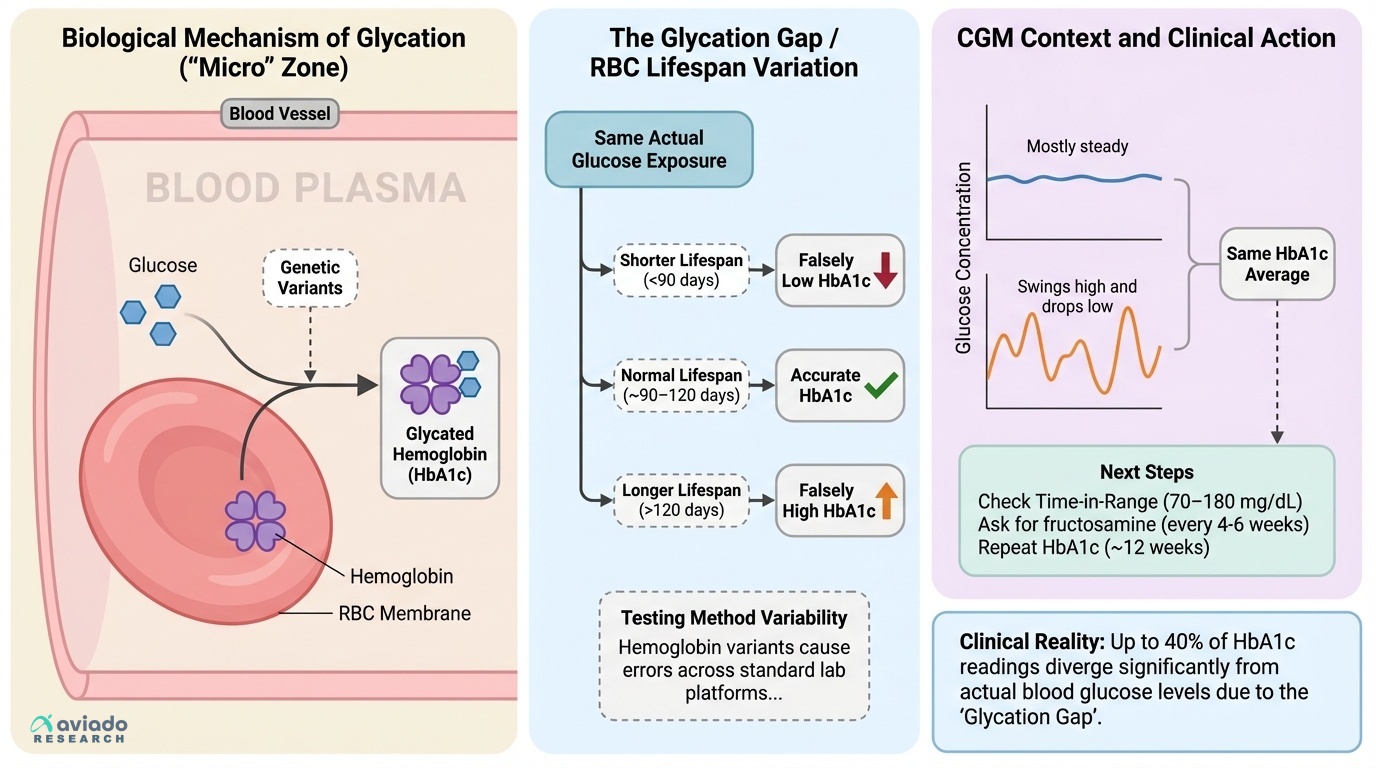
It is surprising, but your HbA1c can mislead you. Most people treat it like a true 3-month average. But your red blood cells can live shorter or longer. That shifts your HbA1c, even at the same glucose.
This means your “good” or “bad” HbA1c may not match you. You can feel fine, see normal meter logs, and still get a high HbA1c. Or the opposite can happen. If your HbA1c and your real glucose disagree, ask for a cross-check.
Use these numbers to guide your next steps. If CGM and HbA1c eAG differ by over 15 mg/dL, dig deeper. Aim for at least 70% time-in-range (70–180 mg/dL). Ask for fructosamine every 4–6 weeks during changes. Repeat HbA1c about every 12 weeks.