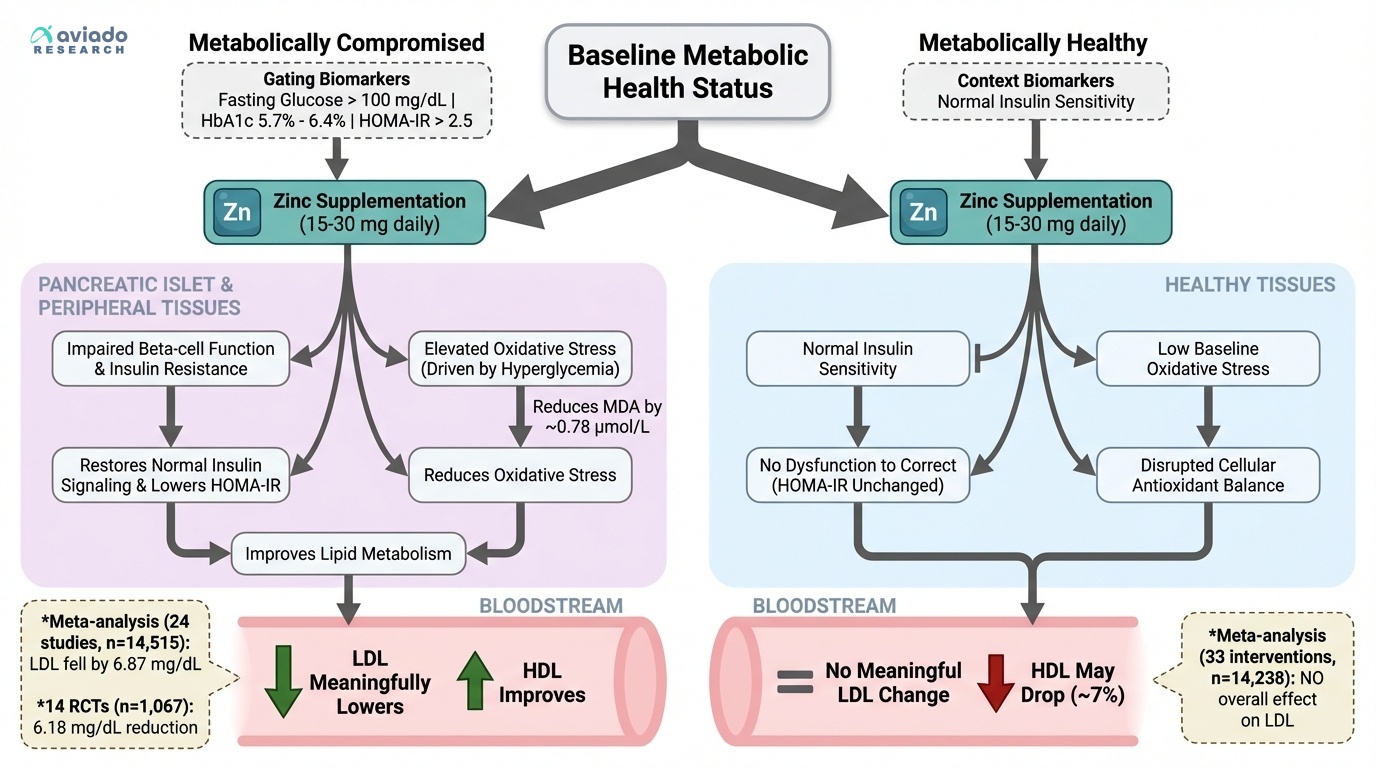
The surprising truth is zinc does not lower cholesterol for everyone. Many people take zinc and expect a sure LDL drop. But the studies split in two. Zinc helps most when your metabolism is already strained.
What this means for you: check your metabolic health first. If you have insulin resistance, prediabetes, or type 2 diabetes, zinc may lower your LDL. If your labs look normal, zinc may do nothing. It may even lower your HDL.
Start with numbers, not guesses. If your fasting glucose is over 100 mg/dL, you may benefit. If your HbA1c is 5.7% to 6.4%, you may benefit. If your HOMA-IR is above 2.5, you may benefit. Typical doses in trials are 15 to 30 mg zinc daily. Recheck lipids after 10 to 12 weeks. Avoid over 40 mg per day long term.