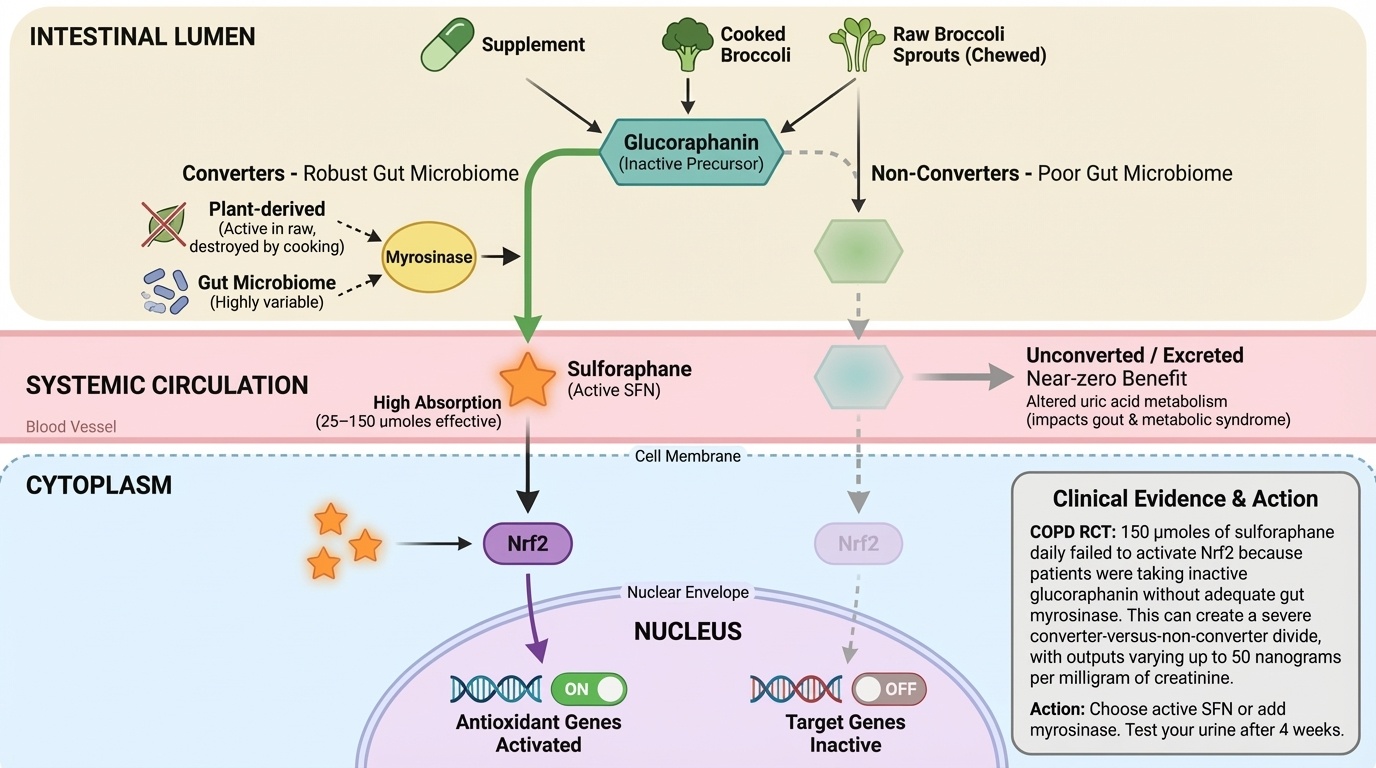
Here's something surprising: most people taking broccoli sprout supplements get almost zero active sulforaphane. The problem is an enzyme called myrosinase. Without it, your body can't convert the inactive stuff in broccoli (glucoraphanin) into the active compound that actually helps you.
This matters because myrosinase gets destroyed by cooking and processing. Most supplements don't include it. Your gut bacteria might do the job instead, but that varies wildly between people. Two people can take identical supplements and get completely different results—sometimes ten times apart in blood levels.
To get real benefits, you need 25 to 150 micromoles of active sulforaphane daily. Choose supplements that contain actual sulforaphane (not just glucoraphanin) or ones that add myrosinase enzyme. Fresh broccoli sprouts work if you chew them raw. Test your urine after 4 weeks to see if it's working—don't just hope.